Alternative Names: Partial Knee Replacement, Unicondylar Knee Replacement, Unicompartmental Knee Replacement, Unicompartmental Knee Arthroplasty, Minimally Invasive Partial Knee Replacement
More than 500,000 people in the United States undergo total knee replacement each year. Some of these patients and an additional gorup of other indivudals with knee arthritis might be candidates for partial knee replacement.
Knee Anatomy
Three bones join together to form the knee joint
· Thighbone (femur)
· Shinbone (tibia)
· Kneecap (patella)
The knee components are held together by muscles, ligaments, and soft tissue. The shock-absorbing material inside the joint that cushions during weight-bearing activities is called the cartilage.
The knee is comprised of three separate section:
· The medial compartment (inside part of the knee)
· The lateral compartment (outside part of the knee)
· The patellofemoral compartment (front part of knee between the kneecap and thigh bone)
Knee Arthritis
Osteoarthritis, or wear-and-tear arthritis, often results in symptoms such as stiffness, pain, and/or a sensation that the knee has “locked” during walking or other activity. The cartilage in the knee degenerates over time until the surfaces are rubbing directly with each other without any cushioning (bone on bone).
Rheumatoid arthritis is an inflammatory process resulting in damage to the surface of the knee joint. Partial knee replacement (PKR) is not indicated in rheumatoid arthritis.
Unicompartmental arthritis is wear and tear disease that affects only one of the three compartments of the joint instead of the entire knee.
Partial Versus Total Knee Replacement
Knee replacement surgery is intended to relieve knee pain and to imporve the function and motion of the knee.
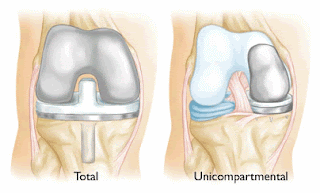
A total knee replacement (TKR) involves the complete repalcement of all three components in the knee. Unicompartmental, or partial knee replacement, allows the surgeon to resurface (or replace) only the damaged compartment of the knee while preserving the health y bone in the other two compartments.
Patients suffering from osteoarthritis that is isolated to only one part/compartment of the knee might be candidates for partial knee replacement. The healthy parts remain untouched during the surgery. Patients also have the opportunity to undergo a standard total knee replacement in the future if the arthritis progresses and additional surgery is needed.
Historical Perspective
Partial knee replecement actually predated Total Knee Replacement. In the 1960’s when the idea of resurfacing an arthritic knee joint was first successfully accomplished, it was with a partial design. It was only after the intial success of these designs that surgeon developers linked together two partials to make the first “Total Knee”-- the Duopatellar. Over the years “total” knee designs have become more and more anatomic following the lead of nature. At the same time partial knee replacement was overshadowed by the success of the “total” design despite the fact that it works so well in certain circumstances. The continued improvement in material science has increased the longevity of both partial and total knee components. Partial knee replacement, when applied to the correct patient, can have superior fuctional results when compared to”total” knee replacement. The operative procedure remains more technically demanding for the surgeon, and is therefore usually provided only by orthopedic surgeons who are Joint Replacement Specialists.
The Procedure
Although the surgeon is able to predict with a high degree of accuracyby review of the x-ray if a patient is a candidate for PKR, the first step in the actual surgical procedure is to examine the three compartments of the knee directly to verify that cartilage damage is present in only one compartment of the knee. If the damage is more significant than was visible on the preoperative x-ray, the surgeon will perform a total knee replacement instead. He or she will discuss this possibility during the preoperative visit.
The term minimally invasive is often thought to relate to incision size. In the hands of a skilled surgeon, the incision size is approximately half the size of the incision made during total knee replacement. In terms of a partial knee replacement, the descripion of minimally invasive also correlates most closely to:
· Preservation of two of the three compartments in the knee joint
· Preservation of the stabilizing ligaments of the knee
o Anterior cruciate ligament (ACL)
o Posterior cruciate ligament (PCL)
During total knee replacement surgery these ligaments are usually cut or loosened. Keeping these intact helps retain a more normal sensation of movement and range of motion.
If the intraoperative examination supports partially resurfacing the knee:
· The damaged bone is removed and replaced with implants (prostheses) made of plastic and metal
· The ends of the thigh and shin bones are cut and reshaped
· The metal implants are secured in place with a fixative substance called bone cement
· A plastic insert is placed between the two metal components to enable the surfaces to freely glide
Advantages of PKR
· Quicker recovery and return to normal activities of daily living
· Smaller incision
· No disruption of the knee cap
· Less pain
· Improved range of motion
· Little to no blood loss
· Reports of a more natural feel in the knee
Disadvantages of PKR
· Potential for additional surgery in the future (if other compartments become damaged by osteoarthritis)
As possible with any surgical procedure, complications can rarely develop:
· Blood clots
· Infection
· Nerve injury
· Persistent pain
· Implant failure
Activity
Most patients can resume normal activities after partial knee replacement when they have regained adequate strength and flexibility. Most exercise and activity are acceptable after surgery including walking, swimming, biking, gardening. Activities that result in repetitive joint trauma such as running, jumping, or twisting should be avoided.
Conclusion
Partial knee replacement can achieve excellent results when performed on the appropriate population of patients. This procedure may be an option for patients who are experiencing significant lifestyle limitations as the result of osteoarthritis isolated to one part of the knee.
If you believe that you may be a candidate for PKR talk to your doctor to determine what treatment is best for you. Since this procedure is technically more challenging and surgeon experience is a key driver of positive surgical outcomes, don’t be hesitant to discuss with your surgeon his or her experience with this procedure.
References
Berger RA, Meneghini RM, Jacobs JJ, et al. Results of unicompartmental knee arthroplasty at a minimum of ten years of follow-up. Journal Bone Joint Surgery Am. 2005; 87(5): 999-1006.